Chronic Diarrhoea
Chronic diarrhoea may be defined as the abnormal passage of 3 or more loose or liquid stools per day for more than 4 weeks
Please refer if likely organic (as opposed to a functional) diarrhoea
- age 45 and over at onset
- nocturnal / continuous (as opposed to intermittent) diarrhoea
- weight loss
- absence of abdominal pain
- rectal bleeding
- abnormal investigations
- family history of GI disease
Consider IBS (functional diarrhoea) in patients if
- abdominal pain, bloating and a change in bowel habit
- age < 45 years old at onset
- no alarm features
- no weight loss
- no nocturnal or continuous (as opposed to intermittent) diarrhoea
- normal investigations (FBC CRP Coeliac screen)
Investigations prior to referral
- Stool MCS
- FBC UE LFT BONE TFT CRP
- coeliac serology
- B12 folate ferritin
2 week wait criteria
Upper GI red flags/2ww criteria:
Refer for direct access gastroscopy:
- Dysphagia
-
Aged 55 or over with weight loss AND any of the following:
- Reflux
- Abdominal pain
- Dyspepsia
Refer to the upper GI 2ww service:
- Ultrasound indicates gall bladder cancer
- CT indicates pancreatic cancer
- Ultrasound indicates pancreatic cancer
- Upper abdominal mass consistent with gastric cancer
- Any patient with jaundice
-
Aged 60 or over with weight loss AND any of the following:
- Diarrhoea
- Back pain
- Abdominal pain
- Nausea
- Vomiting
- Constipation
- New onset diabetes
Lower GI red flags/2ww criteria:
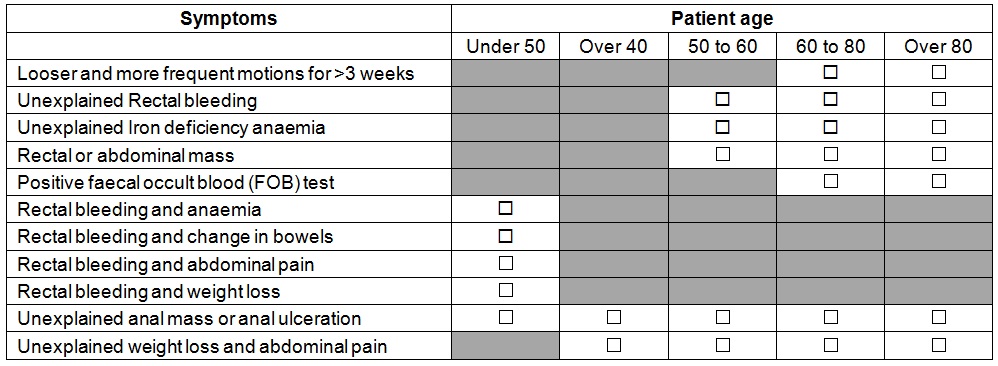
Clinics available
Diarrhoea or change in bowel habit +/- pain Age<45 OP medical
Age >45 OP colorectal/lower GI medical unless 2ww
Referrals for IBS will be rejected if primary care management is incomplete
Reference/Further Reading
http://patient.info/doctor/chronic-diarrhoea-in-adults
British Society of Gastroenterology. Guidelines for the investigation of chronic diarrhoea 2003:
